You’ve been feeling unusually exhausted despite getting enough sleep, your joints ache without explanation, and your skin seems to be developing a strange bronze tint—but you can’t pinpoint why. For thousands of women, these puzzling symptoms point to a serious but often overlooked condition: iron overload. Unlike iron deficiency, which dominates women’s health discussions, high iron levels in women develop silently over decades, accumulating in vital organs until symptoms finally emerge—often at a stage when significant damage has already occurred. Understanding the symptoms of high iron levels in women is critical for early detection, as untreated hemochromatosis can lead to irreversible liver damage, diabetes, heart failure, and other life-threatening complications.
Women face unique challenges with iron overload due to physiological factors that both delay symptom onset and alter the condition’s presentation. The same menstrual cycles and pregnancies that protect women from iron deficiency during their reproductive years also mask early signs of overload, meaning many women remain undiagnosed until after menopause when symptoms suddenly accelerate. This comprehensive guide explores the full spectrum of symptoms of high iron levels in women, from subtle early warnings to serious complications, helping you recognize when to seek medical evaluation and potentially prevent permanent organ damage.
Why Your Fatigue Won’t Go Away Despite Rest
Persistent exhaustion that doesn’t improve with sleep should raise red flags about your iron levels. Women with high iron levels frequently describe a profound, systemic fatigue that makes even simple daily tasks feel overwhelming. This isn’t ordinary tiredness—it’s a deep-seated weakness that lingers regardless of how much you rest. The culprit? Excess iron deposits interfering with cellular energy production throughout your body.
How Iron Overload Fatigue Differs From Normal Tiredness
Normal fatigue typically resolves with adequate rest and sleep, while iron-related fatigue persists despite proper rest and often worsens over time. You might notice:
- Morning exhaustion that doesn’t improve after breakfast
- Difficulty concentrating or “brain fog” that affects work performance
- Needing frequent naps that don’t provide lasting relief
- Physical weakness that makes climbing stairs or carrying groceries challenging
This specific fatigue pattern occurs because excess iron creates oxidative stress in your cells, disrupting mitochondrial function—the very power plants of your body. If you’re experiencing persistent fatigue alongside other unexplained symptoms, request iron studies during your next doctor’s visit—don’t dismiss it as just “getting older.”
Menstrual Changes That Signal Iron Overload
Women with high iron levels often experience significant disruptions to their menstrual cycles long before other symptoms appear. Your periods might become irregular or stop completely, even if you’re still in your reproductive years. This occurs because excess iron accumulates in your pituitary gland and ovaries, interfering with the delicate hormonal balance that regulates menstruation.
Critical Warning Signs in Your Cycle
Missing periods after age 30 with no other explanation could indicate iron overload, especially if accompanied by other symptoms. Women with hemochromatosis frequently report:
- Gradually lighter periods that eventually stop
- Unpredictable cycle lengths with no consistent pattern
- Complete cessation of menstruation (amenorrhea) while still premenopausal
- Sudden changes in flow intensity without hormonal explanation
Don’t assume irregular periods are just stress-related—document your cycle changes and discuss iron testing with your gynecologist, particularly if you have a family history of hemochromatosis or liver disease.
The Postmenopausal Symptom Explosion
If you’re experiencing sudden, unexplained health issues after menopause, high iron levels could be the culprit. The disappearance of monthly blood loss removes your body’s primary mechanism for iron regulation, causing previously silent accumulation to accelerate dramatically. Many women report what feels like abrupt symptom onset in their 50s and 60s, when in reality iron has been building for decades.
Recognizing the Shift From Silent to Symptomatic
Within 1-3 years after menopause, women with undiagnosed hemochromatosis often notice:
- Rapidly worsening fatigue that wasn’t present before
- New joint pain particularly in the knuckles of your hands
- Unexplained abdominal discomfort in the upper right quadrant
- Skin changes including unusual bronze or gray discoloration
This postmenopausal symptom surge explains why women are often diagnosed decades later than men—knowing this timeline helps you advocate for appropriate testing when symptoms emerge after reproductive years end.
Hand Pain That Mimics Arthritis
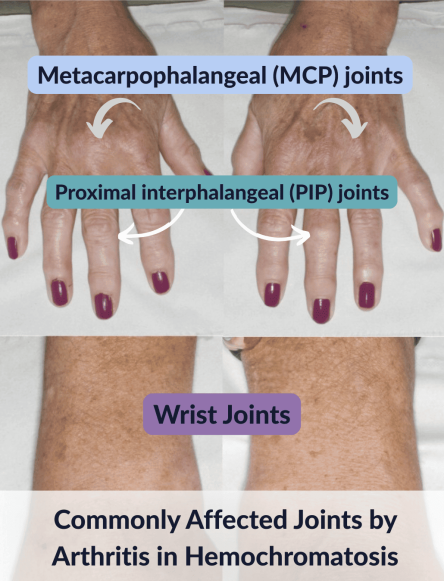
One of the most distinctive early joint symptoms of high iron levels in women targets your hands in a specific pattern. You might experience stiffness, swelling, and pain in the knuckles closest to your fingertips (second and third metacarpophalangeal joints), making everyday tasks like opening jars or writing increasingly difficult.
Differentiating Iron-Related Joint Pain From Arthritis
Hemochromatosis arthropathy has telltale characteristics:
- Pain often appears suddenly in midlife rather than gradually
- Morning stiffness may not improve with activity like typical arthritis
- Symmetrical involvement—both hands affected similarly
- Limited response to standard arthritis treatments
Track your hand pain patterns carefully—if over-the-counter arthritis medications provide little relief and you notice the distinctive knuckle involvement, request iron studies alongside standard rheumatoid factor testing.
Bronze Skin Discoloration: Your Body’s Warning Sign

As iron overload progresses, your skin may develop a distinctive bronze, gray, or tan hue that becomes most noticeable in areas exposed to friction or sun. This hyperpigmentation results from excess iron stimulating increased melanin production while simultaneously depositing iron-storage proteins in your skin cells.
Where to Check for Iron-Related Skin Changes
Examine these areas for telltale discoloration:
- Armpits and groin—often the first places bronze discoloration appears
- Inside old scars—iron deposits concentrate in scar tissue
- Backs of hands and forearms—particularly noticeable compared to covered areas
- Sun-exposed regions—face, neck, and chest showing uneven darkening
Don’t mistake this for normal tanning—bronze hyperpigmentation from iron overload develops gradually over months or years and doesn’t fade when sun exposure decreases. Document any skin color changes with photos to show your doctor.
Liver Warning Signs You Shouldn’t Ignore
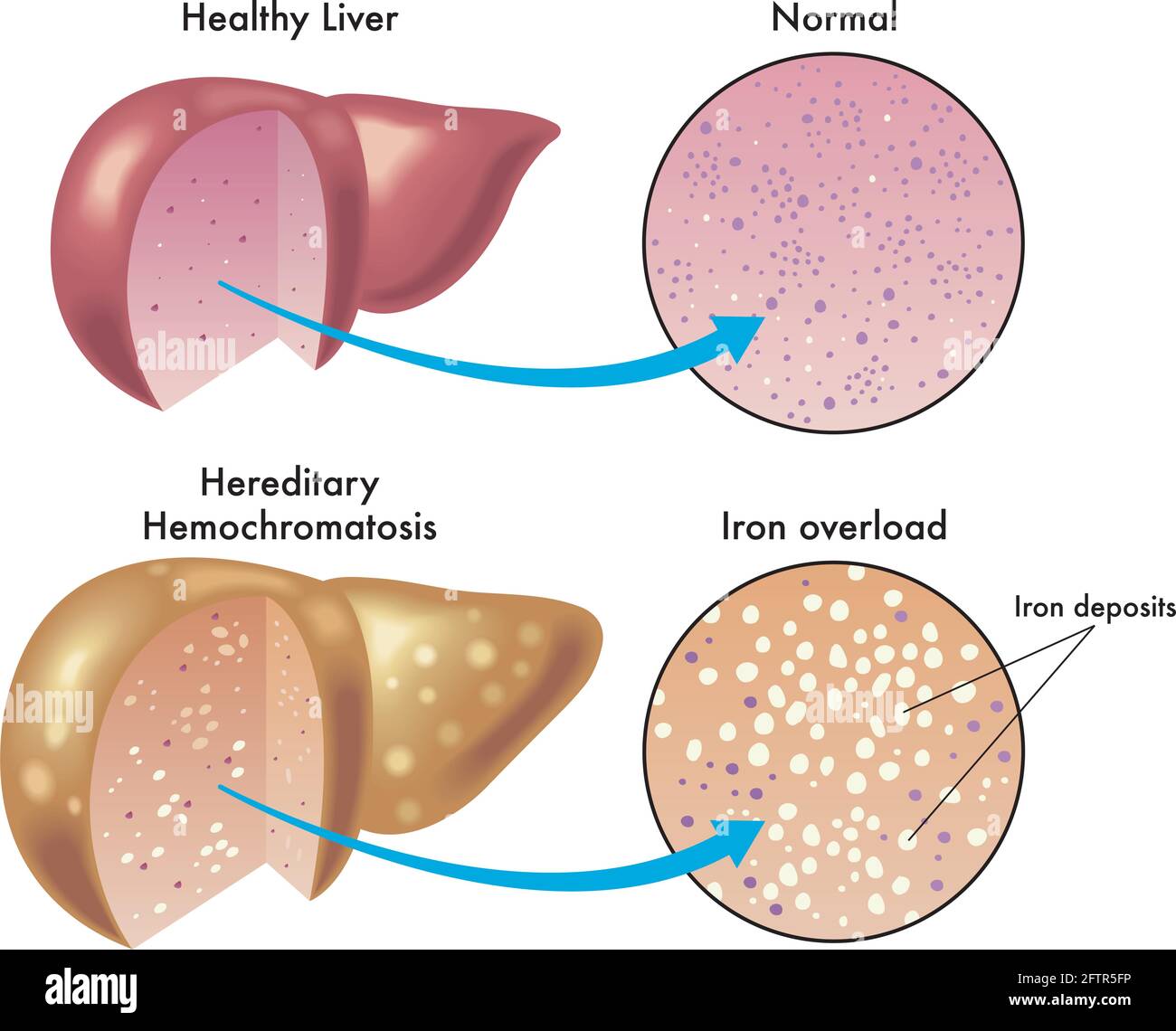
Your liver bears the brunt of iron overload, storing up to 70% of excess iron in your body. As iron accumulates, it causes inflammation and scarring that may initially produce subtle symptoms but can progress to serious complications like cirrhosis and liver cancer.
Early Liver Distress Signals
Watch for these often-overlooked indicators of liver involvement:
- Persistent upper right abdominal discomfort—a feeling of fullness or mild pain
- Unexplained nausea especially after fatty meals
- Itchy skin without rash—caused by bile buildup from impaired liver function
- Easy bruising from reduced production of clotting proteins
If you experience these symptoms alongside fatigue or joint pain, request both liver function tests AND iron studies—standard liver panels alone won’t detect iron overload as the underlying cause.
The Diabetes Connection You Need to Know
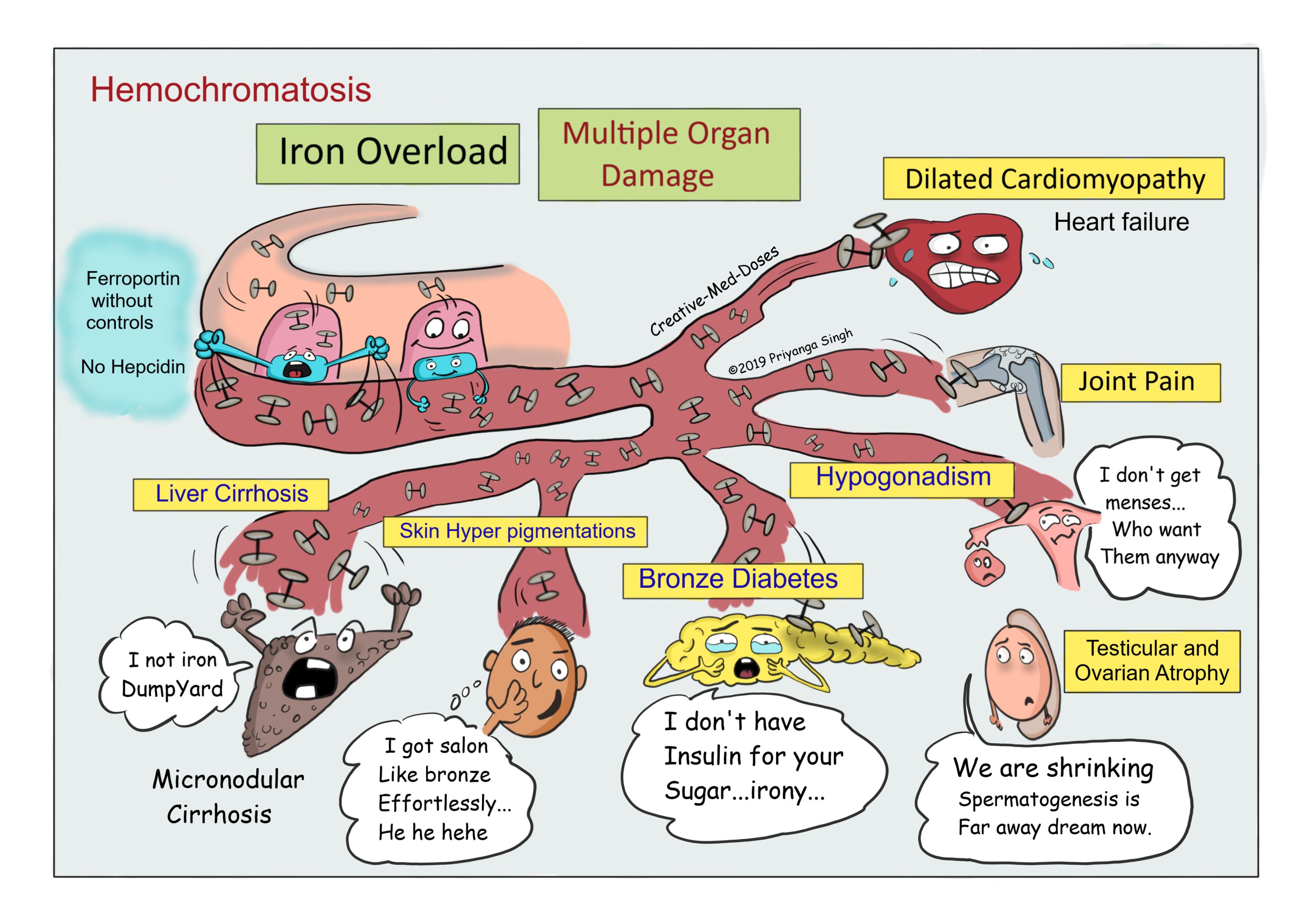
Women developing diabetes after age 40 without typical risk factors should consider high iron levels as a potential cause. Iron deposits in the pancreas damage insulin-producing beta cells, leading to what’s clinically known as “bronze diabetes” when it occurs with hemochromatosis.
Recognizing Iron-Related Blood Sugar Issues
Symptoms that might indicate iron-induced diabetes include:
- Rapidly progressing blood sugar problems despite standard management
- Unexplained weight loss while eating normally
- Extreme thirst and frequent urination appearing suddenly
- Darkened skin accompanying new diabetes diagnosis
If you’ve been diagnosed with diabetes but don’t fit the typical profile, ask your doctor about iron testing—managing the underlying iron overload may improve your diabetes control.
When to Demand Iron Testing From Your Doctor
Many women suffer for years with undiagnosed iron overload because symptoms get misattributed to aging or stress. Knowing when to advocate for specific testing could prevent irreversible organ damage.
Must-Request Tests If You Have These Risk Factors
Ask for serum ferritin and transferrin saturation tests if you experience:
- Persistent fatigue unexplained by other causes
- Hand joint pain with the distinctive knuckle pattern
- Unexplained liver enzyme abnormalities
- New-onset diabetes without obesity or family history
- Family history of hemochromatosis, liver disease, or early heart disease
- Postmenopausal women with any combination of these symptoms
Don’t accept “normal” iron tests without context—ferritin levels above 300 ng/mL in postmenopausal women or transferrin saturation over 45% warrant further investigation, even if your doctor says results are “within normal range.”
Action Plan for Women Suspecting Iron Overload
If you recognize these symptoms in yourself, take these immediate steps to protect your health:
- Document your symptoms with specific dates, severity, and patterns
- Research your family history—hemochromatosis affects multiple relatives
- Request specific iron studies (ferritin and transferrin saturation) at your next appointment
- Avoid iron supplements and vitamin C with meals until you have test results
- Limit alcohol consumption which accelerates iron-related liver damage
Early diagnosis before significant organ damage occurs offers dramatically better outcomes—women who begin treatment while still asymptomatic can prevent nearly all complications of hemochromatosis.
Critical Prevention Strategies After Diagnosis
If testing confirms high iron levels, these evidence-based approaches will protect your organs:
- Commit to regular phlebotomy—weekly sessions initially until iron normalizes
- Avoid iron-fortified foods and supplements—read all labels carefully
- Limit red meat and organ meats—choose plant-based iron sources instead
- Drink tea or coffee with meals—polyphenols reduce iron absorption
- Schedule annual screenings for liver, heart, and pancreatic function
With consistent treatment, most women with hemochromatosis live full, healthy lives—the key is catching it before irreversible damage occurs. Recognizing the symptoms of high iron levels in women represents your first step toward taking control of this treatable condition. Don’t dismiss persistent symptoms as “just part of aging”—your future health depends on investigating these warning signs today.





