Finding elevated vitamin B12 levels alongside low iron on your blood test results can be confusing and concerning. Many patients mistakenly assume that high B12 must be beneficial, while low iron explains their fatigue—but this unusual combination often signals something more complex happening in your body. Understanding this paradoxical lab pattern is crucial because it frequently points to underlying conditions requiring medical attention rather than simple nutritional supplementation.
This specific blood work discrepancy affects more people than you might think, yet it’s rarely discussed in mainstream health conversations. When your doctor sees high B12 with low iron, they’re immediately alerted to potential issues with your liver, bone marrow, or immune system—not just dietary deficiencies. The relationship between these two nutrient markers creates a diagnostic puzzle that, when solved correctly, can reveal serious health conditions before more obvious symptoms develop.
In this guide, you’ll discover why these seemingly unrelated nutrient abnormalities often appear together, what medical conditions commonly cause this pattern, and how healthcare providers determine the underlying cause. Most importantly, you’ll learn why treating just the iron deficiency without addressing the root problem could miss something significant affecting your long-term health.
Liver Disease: The Primary Link to Elevated B12
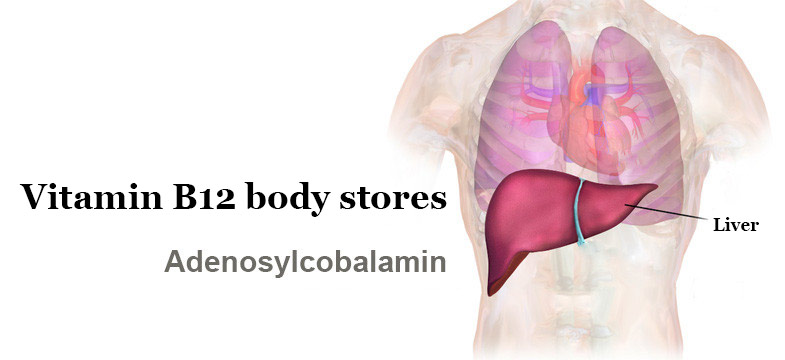
Your liver acts as the body’s main storage facility for vitamin B12, holding significant reserves that get released into circulation when liver cells become damaged or die. This explains why liver conditions represent the most common cause of elevated B12 alongside iron abnormalities. When hepatocytes (liver cells) are injured, they release stored B12 into the bloodstream, creating artificially high readings on standard blood tests.
How Hepatitis Triggers This Lab Pattern
Viral hepatitis (such as hepatitis B or C), alcoholic hepatitis, and autoimmune hepatitis all damage liver tissue, causing stored B12 to flood into circulation. At the same time, chronic inflammation from hepatitis disrupts iron metabolism, leading to functional iron deficiency. You might notice symptoms like fatigue that seems disproportionate to your activity level, right upper abdominal discomfort, or unexplained jaundice (yellowing of skin and eyes).
Cirrhosis and Nutrient Processing Failure
In advanced cirrhosis, the liver’s ability to process and regulate nutrients becomes severely compromised. While B12 levels rise due to cellular damage, iron metabolism falters—sometimes showing as low iron due to impaired transport, or paradoxically high iron if the cirrhosis stems from hemochromatosis. Patients with cirrhosis often experience easy bruising, abdominal swelling, and confusion alongside these lab abnormalities.
Non-Alcoholic Fatty Liver Disease Connection
NAFLD affects nearly 25% of adults worldwide and frequently produces this exact lab pattern. As fat accumulates in liver cells and inflammation develops, the organ’s nutrient regulation systems malfunction. What makes NAFLD particularly concerning is that patients often show no obvious symptoms until significant damage has occurred, making these blood test abnormalities an important early warning sign.
Autoimmune Conditions Creating Confusing Lab Results
Autoimmune disorders frequently generate laboratory patterns that seem contradictory at first glance, and high B12 with low iron fits this category perfectly. These conditions create systemic inflammation that simultaneously disrupts multiple bodily systems responsible for nutrient processing.
Pernicious Anemia’s Paradoxical Presentation
While pernicious anemia typically causes B12 deficiency, the autoimmune attack on stomach cells can sometimes produce elevated B12 during active inflammation phases before deficiency develops. This happens because damaged parietal cells release stored B12 while simultaneously impairing future absorption. Patients might experience burning tongue, neurological symptoms, and profound fatigue that doesn’t improve with iron supplements alone.
Lupus and Rheumatoid Arthritis Impact
Systemic autoimmune conditions like lupus and rheumatoid arthritis trigger inflammatory cytokines that signal the body to sequester iron away from circulation—a defense mechanism against pathogens that starves bacteria of essential nutrients. This creates “anemia of chronic disease” with low available iron, while concurrent autoimmune hepatitis or liver involvement elevates B12 levels. Joint pain, morning stiffness, and unexplained fevers often accompany these lab findings.
Blood Disorders That Alter Nutrient Metabolism
Bone marrow abnormalities directly impact how your body handles both iron and B12 since these nutrients work together in red blood cell production. When blood cell formation becomes dysregulated, laboratory patterns frequently include elevated B12 with depleted iron stores.
Myeloproliferative Disorders Explained
Conditions like polycythemia vera cause the bone marrow to overproduce blood cells, increasing production of transcobalamin (the protein that transports B12) and raising circulating levels. Simultaneously, rapidly dividing cells consume iron at accelerated rates, depleting stores. Patients might notice headaches, dizziness, itching after showers, or blood clots alongside these lab abnormalities.
Chronic Leukemia’s Dual Impact
Chronic myelogenous leukemia (CML) disrupts normal blood cell production through multiple mechanisms. Increased cellular turnover releases stored B12 while abnormal cell populations consume excessive iron. Unexplained weight loss, night sweats, and abdominal fullness from an enlarged spleen often signal this condition before blood tests reveal the high B12/low iron pattern.
Medication Side Effects You Should Know

Several common medications can create this laboratory pattern either directly or through the conditions they treat. Recognizing these medication effects prevents unnecessary testing and ensures proper treatment.
Diabetes Medication Complications
Metformin, the first-line treatment for type 2 diabetes, typically reduces B12 absorption—but paradoxically, some long-term users show elevated levels. This likely reflects underlying diabetic complications affecting the liver rather than the medication itself. Meanwhile, diabetes-related kidney disease contributes to iron deficiency through multiple mechanisms including chronic blood loss during dialysis.
Acid-Reducing Medications and Nutrient Processing
Proton pump inhibitors (PPIs) like omeprazole reduce stomach acid needed for B12 release from food proteins. While this usually causes deficiency, some patients show elevated levels due to concurrent conditions. More significantly, long-term PPI use impairs iron absorption, creating the low iron component of this pattern. Consider discussing periodic medication holidays with your doctor if you’ve been on PPIs for years.
Interpreting Your Specific Lab Values
Understanding the numerical significance of your results helps determine urgency and appropriate next steps. Not all elevated B12 levels carry equal concern.
What Your B12 Numbers Really Mean
Values significantly above 900 pg/mL—especially exceeding 1500—strongly suggest liver disease or malignancy rather than dietary excess. Mild elevations between 900-1200 require clinical context for interpretation. If your B12 measures 1800 pg/mL with ferritin under 15 ng/mL, this combination warrants immediate investigation.
Iron Study Breakdown
Ferritin (iron stores) below 15 ng/mL confirms true iron deficiency, while transferrin saturation under 20% indicates functional deficiency. When both appear alongside elevated B12, autoimmune or liver disease becomes highly likely. Your healthcare provider should also check CRP or ESR to assess inflammation levels.
Critical Symptoms That Demand Immediate Attention
While some causes develop gradually, certain symptom combinations require prompt evaluation to rule out serious conditions.
Warning Signs Beyond Fatigue
Seek immediate medical attention if you experience unexplained weight loss exceeding 10 pounds in 6 months, persistent abdominal pain that worsens after eating, easy bruising without injury, or neurological symptoms like numbness or balance problems alongside this lab pattern. These could indicate progressing liver disease or hematologic malignancy.
When Iron Supplements Don’t Help
If you’ve been taking iron supplements for months without symptom improvement—despite normalizing your iron levels—this strongly suggests an underlying condition preventing proper iron utilization. Your doctor should investigate why your body isn’t using the supplemented iron effectively.
Treatment Approaches That Address the Real Problem
Effective management focuses on the underlying condition rather than just correcting the lab abnormalities.
Liver Disease Management Strategies
For NAFLD-related patterns, weight loss of 5-10% often significantly improves liver function and normalizes both B12 and iron levels. Alcohol cessation is non-negotiable for alcohol-related liver disease. Antiviral therapy for hepatitis can resolve the lab abnormalities within months of successful treatment.
Autoimmune Condition Protocols
Immunosuppressive therapy for autoimmune hepatitis typically normalizes both elevated B12 and iron metabolism within 6-12 months of achieving remission. For lupus-related patterns, controlling systemic inflammation with appropriate medications allows iron metabolism to return to normal.
When to Request Specialist Referral
Not all primary care providers recognize the significance of this lab pattern. Knowing when to seek specialist care ensures timely diagnosis.
Hepatology Consultation Triggers
Request a hepatology referral if you have elevated liver enzymes (ALT, AST) alongside this pattern, especially if they remain abnormal after 8-12 weeks. Persistent B12 elevation above 1200 pg/mL with low iron also warrants specialist evaluation to rule out serious liver conditions.
Hematology Assessment Indicators
See a hematologist if you have abnormal blood counts (beyond simple anemia), unexplained blood clots, or symptoms like night sweats and bone pain. These suggest possible bone marrow disorders requiring specialized evaluation.
The high B12 and low iron pattern serves as an important medical clue rather than a diagnosis itself. By understanding this connection, you become an informed partner in your healthcare journey—able to ask the right questions and ensure proper investigation of potentially serious underlying conditions. Never dismiss this combination as merely “needing iron supplements”; it represents your body’s way of signaling that something fundamental requires attention. Work with your healthcare provider to systematically investigate possible causes, as early intervention often leads to better outcomes for the conditions driving this unusual laboratory pattern.