Iron supplements rank among the most commonly prescribed treatments for iron deficiency anemia, yet they come with a notorious reputation for causing stomach upset. If you’ve started taking iron pills only to find yourself racing to the bathroom or feeling perpetually queasy, you’re far from alone. Recent studies indicate that up to 70% of people taking standard iron supplements experience some form of gastrointestinal distress, with nausea being the most commonly reported symptom. The frustrating irony is that the very medication meant to restore your energy and health can leave you feeling worse than before you started.
The good news is that nausea from iron pills doesn’t have to derail your treatment. Most people successfully manage these symptoms through simple adjustments to how, when, and what form of iron they take. This guide walks you through proven strategies to stop nausea from iron pills while still getting the therapeutic benefit your body needs. By the end, you’ll have a complete toolkit for making iron supplementation tolerable and effective—without compromising your treatment for iron deficiency.
Why Iron Pills Cause Nausea
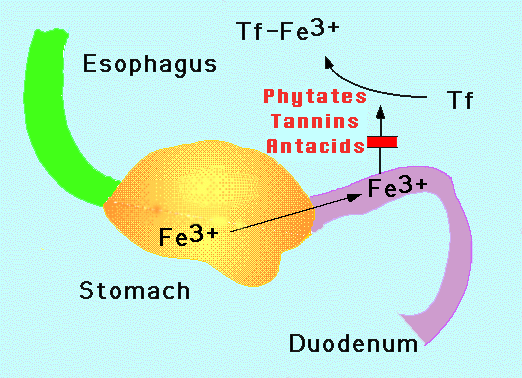
Understanding what triggers your nausea gives you power over it. Iron supplements cause gastrointestinal distress through several mechanisms, and recognizing which applies to your situation helps you choose the most effective remedy.
Iron is inherently irritating to the stomach lining. When you swallow an iron tablet, it dissolves in your digestive tract, releasing free iron ions that can directly irritate the stomach mucosa. This irritation triggers the nausea reflex as your body signals that something uncomfortable is happening internally. The effect intensifies with higher doses, which is why taking a full 325-milligram ferrous sulfate tablet (the most common prescription strength) often produces stronger symptoms than lower doses.
The chemical form of iron matters significantly. Ferrous sulfate, the most frequently prescribed form, contains a moderate amount of elemental iron per tablet but tends to cause more stomach upset than other formulations. Ferrous gluconate contains less elemental iron per dose but is generally gentler on the stomach, while ferrous fumarate delivers the highest concentration of elemental iron in each tablet. Individual tolerance varies considerably—some people tolerate one form perfectly well while experiencing severe nausea with another.
Timing and stomach contents also play crucial roles. Iron absorbs most efficiently on an empty stomach, but this optimal absorption comes at the cost of increased irritation. When you take iron with food, absorption decreases somewhat, but so does the likelihood of nausea. Finding your personal sweet spot between absorption and tolerance requires some experimentation, though the strategies in this guide can accelerate that process.
Take Iron with Food Strategically
The most immediately effective approach to reducing iron-induced nausea involves taking your supplement with food—but not just any food, and not arbitrarily. Strategic food timing transforms this simple solution from a guess into a precise intervention.
Starting with a small amount of food provides the greatest benefit for the least absorption cost. A few crackers, a slice of bread, or a small serving of oatmeal creates a protective buffer in your stomach without dramatically reducing iron uptake. The food absorbs some of the direct iron contact with your stomach lining while still allowing sufficient absorption through the intestinal wall. This compromise works well for many people who experience mild to moderate nausea.
Certain foods act as absorption blockers and must be avoided when taking iron. Calcium stands as the most significant culprit—milk, cheese, yogurt, and calcium-fortified products all interfere dramatically with iron absorption. Wait at least two hours after consuming any calcium-containing food before taking your iron supplement. Similarly, antacids (including Tums, Rolaids, and Maalox) neutralize stomach acid needed for iron dissolution and should never be taken concurrently with iron pills.
Caffeine and high-fiber foods present additional challenges. Coffee, tea, energy drinks, and even chocolate contain compounds that bind iron and prevent its absorption. Whole grains, raw vegetables, and bran products contain phytates and fiber that similarly interfere with iron uptake. You don’t need to eliminate these foods entirely from your diet, but timing matters considerably—consume them several hours before or after your iron dose rather than alongside it.
Adjust Your Dosage and Form

When dietary modifications prove insufficient, dosage and formulation changes often provide the breakthrough you need. These adjustments require consultation with your healthcare provider, but the effort typically pays off in dramatically improved tolerability.
Splitting your daily dose into smaller, more frequent administrations reduces the peak concentration of iron in your digestive tract at any one time. Rather than taking one 325-milligram tablet, your doctor might recommend taking half that dose twice daily or even smaller amounts spread throughout the day. This approach maintains the same total daily iron intake while giving your stomach less irritant to process at once. Many people find that this simple change eliminates nausea entirely.
Different iron formulations offer different tolerability profiles. If ferrous sulfate consistently causes problems, asking your healthcare provider about switching to ferrous gluconate or ferrous fumarate makes sense. These alternative forms contain different amounts of elemental iron per dose and have different chemical properties that affect how they interact with your digestive system. Some people discover through trial that one form agrees with them while others don’t—a matter of individual biochemistry rather than any inherent superiority of one form over another.
Liquid iron preparations represent another option for those who cannot tolerate any tablet form. Liquid supplements typically cause less nausea because they distribute more evenly through the digestive system rather than sitting as a concentrated mass in your stomach. The trade-off involves tooth staining, which can be minimized by mixing the liquid with juice or water and drinking through a straw. Any staining that does occur responds well to brushing with baking soda or hydrogen peroxide.
Boost Absorption While Reducing Nausea
Managing nausea often means accepting some reduction in iron absorption, but you can counterbalance this effect through strategic complementary interventions. The goal is getting enough iron into your system despite the compromises necessary to keep nausea at bay.
Vitamin C dramatically enhances iron absorption, sometimes by as much as threefold when taken together. This means that the iron you do absorb while taking your supplement with food can be substantially increased by adding vitamin C to the equation. A simple glass of orange juice (approximately eight ounces) taken with your iron pill provides sufficient vitamin C for this benefit. Alternatively, a vitamin C supplement of 250 to 500 milligrams works equally well. This combination partially offsets the absorption reduction from taking iron with food.
Adequate fluid intake supports both absorption and tolerance. Approximately eight ounces of water or other non-interfering liquids with each iron dose helps move the supplement through your stomach more quickly and reduces direct irritation. The fluid also aids in dissolving the iron tablet and presenting it to your intestinal absorption sites in a more favorable form. Just ensure you’re not drinking milk, caffeinated beverages, or calcium-fortified drinks—plain water, fruit juices, and vegetable juices all work well.
Spacing other medications and supplements appropriately prevents interactions that reduce iron absorption. Thyroid medications, certain antibiotics (particularly tetracyclines and fluoroquinolones), and some osteoporosis medications all compete with iron for absorption. Taking these medications at least two hours apart from your iron supplement ensures each gets a fair opportunity to work.
Manage Additional Side Effects
:max_bytes(150000):strip_icc()/do-iron-supplements-for-anemia-cause-upset-stomach-3522504-01-a8806fc982ab45998d75000e183bc406.png)
Nausea rarely travels alone when it comes to iron supplementation. Understanding and addressing companion symptoms helps you maintain the comprehensive approach necessary for successful long-term treatment.
Constipation affects many iron supplement users and compounds the discomfort of nausea. The iron itself slows digestive transit, and reduced fluid intake (sometimes people drink less to avoid feeling full) worsens the problem. If constipation becomes uncomfortable, a stool softener such as docusate sodium (commonly sold as Colace) provides relief without interfering with iron absorption. Increasing dietary fiber (at times other than your iron dose) and maintaining adequate hydration throughout the day also help keep things moving.
Diarrhea represents the opposite problem, occurring in some people rather than constipation. The same principles apply—staying hydrated matters enormously if you’re experiencing loose stools. Unlike constipation, antidiarrheal medications don’t interfere with iron absorption, so loperamide or similar products can be used if needed. Some people find that switching to a lower-iron formulation or splitting the dose resolves diarrhea issues.
Black or dark green stools might alarm you if you expect them, but this harmless side effect simply reflects unabsorbed iron passing through your digestive tract. The color change has no health implications and provides no useful information about your iron status or absorption. However, black stools combined with other unusual symptoms—particularly severe abdominal pain, vomiting blood, or tarry stools that might indicate gastrointestinal bleeding—warrant immediate medical attention.
When to Contact Your Healthcare Provider
While most iron-related nausea responds well to the strategies outlined above, certain situations require professional medical guidance. Recognizing these scenarios prevents both unnecessary suffering and potential complications.
Persistent vomiting or inability to keep any iron supplement down for more than a few days signals a problem requiring medical attention. Severe nausea that prevents adequate nutrition and hydration threatens your overall health and may indicate that your current approach isn’t working. Your healthcare provider might need to investigate whether an underlying condition contributes to your sensitivity or whether intravenous iron represents a better option for your situation.
Symptoms suggesting an allergic reaction or serious intolerance merit immediate medical evaluation. Difficulty breathing, swelling of the face or throat, hives, or rash developing after starting iron supplementation could indicate an allergic reaction requiring prompt treatment. While true iron allergies are rare, they do occur and require professional diagnosis and management.
Any decision to stop iron supplementation should involve your healthcare provider. Treatment for iron deficiency anemia typically requires continuing supplements for six to twelve months after blood counts normalize to fully replenish bone marrow iron stores. Stopping prematurely because of nausea wastes the investment you’ve already made in your treatment and allows iron deficiency to recur. Your provider can help you find an approach that allows you to complete your treatment successfully.
Quick Reference Tips for Relief
Arming yourself with a consolidated checklist of nausea-prevention strategies helps you implement them consistently and systematically.
Take iron with a small amount of food (crackers, bread, or oatmeal) rather than on an empty stomach or with a full meal. Avoid calcium-containing foods, antacids, caffeine, and high-fiber items for two hours before and after each dose. Consider splitting your total daily dose into smaller portions taken multiple times daily if one dose causes significant nausea. Ask your healthcare provider about alternative iron formulations if your current supplement consistently causes problems. Drink approximately eight ounces of water or juice (not milk or caffeine) with each dose. Add vitamin C through orange juice or a supplement to enhance absorption of iron taken with food. Use a stool softener if constipation becomes problematic, and remember that black stools are normal and harmless. Store iron tablets in a cool, dry place (not the bathroom) and keep them away from children, as iron overdose is dangerous.
Finding the right combination of strategies for your body requires patience and experimentation. What works perfectly for one person may need adjustment for another. The key is approaching the problem systematically—try one change at a time, give it several days to evaluate effectiveness, then move on to the next strategy if needed. Most people successfully achieve a tolerable iron supplementation regimen within a few weeks, allowing them to complete their treatment for iron deficiency anemia without ongoing nausea or other significant side effects.
Your commitment to overcoming iron supplement nausea reflects a broader commitment to your health. Iron deficiency anemia, when left untreated, depletes your energy, impairs your immune function, and can cause serious complications. By taking an active role in managing the side effects of your treatment, you’re investing in your long-term wellness. Use these strategies, work closely with your healthcare provider, and give your body the time it needs to adjust. The temporary inconvenience of managing nausea pays lasting dividends in restored energy and health.