Iron supplements rank among the most commonly used dietary supplements globally, frequently prescribed for iron deficiency anemia and taken by millions who hope to boost their energy and overall health. However, what many people don’t realize is that iron supplementation carries significant risks that can range from mild digestive discomfort to life-threatening poisoning, particularly in children. Research reveals that daily iron intake among supplement users can reach nearly 19 times the recommended daily allowance in some populations—a staggering finding that highlights how easily supplementation can spiral into excess. Understanding these risks before starting an iron supplement regimen isn’t just prudent; it could protect you from serious health consequences that many healthcare providers don’t adequately communicate.
The dangers associated with iron supplements extend far beyond the occasional upset stomach. Scientific research has established clear links between inappropriate iron supplementation and oxidative damage to gastrointestinal tissues, systemic toxicity, dangerous drug interactions, and potential long-term consequences including increased cancer risk. Perhaps most alarming is the fact that iron poisoning remains a leading cause of fatal poisoning in young children, making proper storage and handling absolutely essential for any household containing iron products. This guide examines the complete spectrum of iron supplement risks, from immediate side effects to chronic health implications, providing you with the knowledge needed to make informed decisions about whether iron supplementation is appropriate for your specific situation.
Common Side Effects of Iron Supplements
Nearly everyone who takes iron supplements experiences some degree of adverse effects, though the severity and specific symptoms vary considerably from person to person. Understanding these common side effects helps you distinguish between normal reactions that can be managed and symptoms that warrant immediate medical attention. The frequency and intensity of side effects often correlate with the dose taken, the specific formulation used, and individual factors such as stomach sensitivity and concurrent medication use.
Digestive Problems from Iron Pills
Iron supplements irritate the gastrointestinal tract in the majority of users, manifesting as a constellation of uncomfortable symptoms that can significantly impact quality of life. The most frequently reported issues include stomach pain, heartburn, nausea, and diarrhea, with constipation being paradoxically common despite the diarrhea some experience. This gastrointestinal distress occurs because iron is inherently reactive with the mucosal lining of the digestive system, creating chemical conditions that promote inflammation and irritation. Many patients find that these symptoms persist throughout the entire course of supplementation, which can extend for several months, making adherence to treatment regimens challenging.
The mechanism behind these digestive disturbances involves iron’s tendency to generate reactive oxygen species when it contacts the moist environment of the gastrointestinal tract. This oxidative stress damages the delicate epithelial cells lining the stomach and intestines, triggering inflammatory responses that manifest as pain and discomfort. Research has demonstrated that even a single clinical dose of ferrous sulfate can induce measurable oxidative damage in healthy individuals, confirming that these aren’t merely subjective complaints but represent genuine physiological insult to gastrointestinal tissues.
Managing Constipation and Stomach Issues
Addressing iron-related digestive problems requires strategic approaches that balance symptom management against the need for effective iron absorption. Taking iron with food can substantially reduce gastrointestinal irritation, though this convenience comes at a cost—food, particularly dairy products and beverages containing caffeine, significantly decreases iron absorption efficiency. Healthcare providers often recommend taking iron on an empty stomach when tolerable, switching to food-based dosing only when side effects become unmanageable. Increasing fluid intake and consuming fiber-rich foods like fruits and vegetables can help counteract the constipating effects that many experience, though patients should avoid taking fiber supplements simultaneously with iron as this can further reduce absorption.
The elixir form of iron supplements offers an alternative for those who struggle with tablet-related stomach issues, though this formulation comes with its own precautions. Mixing the elixir with water or fruit juice helps prevent the teeth staining that commonly occurs with liquid iron preparations. Patients should never mix iron elixirs with milk or wine-based solutions, as these substances can interfere substantially with absorption. Using the special dropper that comes with iron drops and asking your pharmacist or physician to demonstrate proper technique ensures accurate dosing and minimizes waste while reducing the risk of accidental staining or ingestion errors.
Gastrointestinal Damage from Iron Supplementation
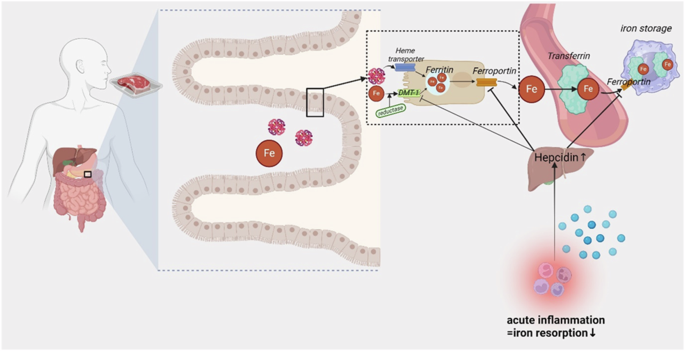
Beyond common side effects, iron supplementation can cause genuine damage to the gastrointestinal tract, ranging from superficial mucosal irritation to ulceration and exacerbation of chronic inflammatory conditions. The research documenting these effects comes from both human clinical studies and animal models, establishing a clear biological basis for concern. Understanding how iron damages gastrointestinal tissues helps patients and providers make informed decisions about supplementation strategies and monitoring requirements.
Ulceration and Tissue Damage
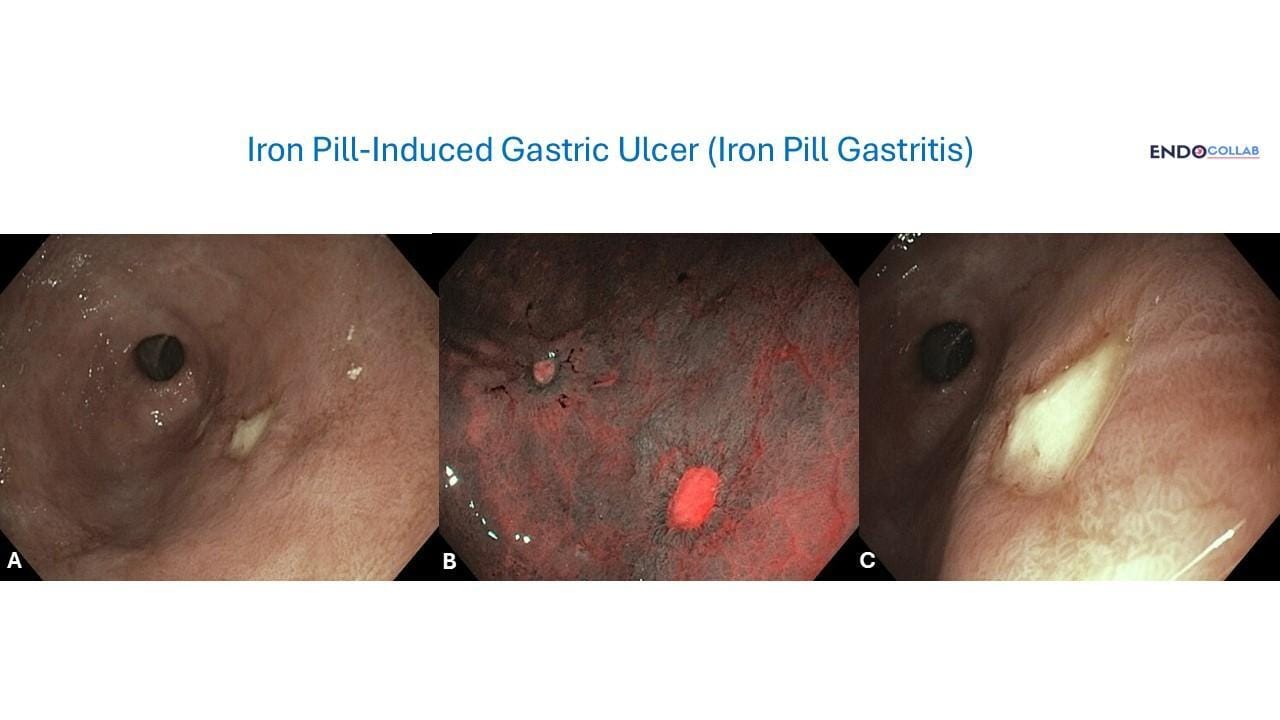
The combination of iron with vitamin C—a pairing commonly recommended to enhance iron absorption—creates a particularly damaging duo for gastrointestinal tissues. Studies have demonstrated that co-supplementation of ferrous salts with vitamin C significantly exacerbates oxidative stress in the gastrointestinal tract, leading to ulceration even in previously healthy individuals. Research using rat models showed that injecting ferrous iron and ascorbic acid in combination produced penetrating gastric ulcers, while neither compound alone caused similar damage when injected into the gastric wall. This finding has profound implications for the widespread practice of recommending vitamin C alongside iron supplements to boost absorption.
The mechanism underlying this damage involves lipid peroxidation mediated by oxygen radicals, a destructive process that breaks down the fatty components of cell membranes and destroys cellular integrity. Treatment with superoxide dismutase, an enzyme that neutralizes certain reactive oxygen species, significantly decreased ulceration in experimental models while simultaneously reducing markers of lipid peroxidation. This confirms that the damage isn’t simply irritation from iron’s direct chemical properties but represents genuine oxidative injury that can be prevented through antioxidant intervention. For patients with pre-existing gastrointestinal conditions, these findings suggest extreme caution is warranted when considering combined iron and vitamin C supplementation.
Iron Poisoning: A Medical Emergency
Acute iron poisoning represents one of the most serious and potentially fatal consequences of iron supplement use, particularly in pediatric populations. Unlike many toxic exposures where effects develop gradually, iron poisoning progresses through distinct stages with increasingly severe manifestations. Recognizing the signs of iron poisoning and responding immediately can mean the difference between full recovery and permanent damage or death.
Why Children Face the Highest Risk

Accidental overdose of iron-containing products remains a leading cause of fatal poisoning in children under six years of age, a distinction that has prompted extensive public health campaigns and regulatory action. The attraction of iron pills to children likely relates to their sugar-coated formulations and the mistaken belief that vitamins are inherently safe. Many households contain adult multiple vitamin supplements that include iron, prenatal vitamins with high iron content, or standalone iron supplements—all representing potential sources of lethal exposure for curious toddlers.
The danger stems from the relatively small body size of young children combined with iron’s dose-dependent toxicity. What constitutes a therapeutic adult dose can represent a massive overdose for a small child. Children’s chewable vitamins, despite containing iron, typically don’t provide enough elemental iron to cause serious poisoning even if an entire bottle is consumed. However, pure iron supplements and prenatal vitamins—which contain substantially higher iron concentrations—can cause serious or fatal poisoning in small children who consume even modest numbers of pills. This distinction makes storage security absolutely critical, as the difference between a child-safe and child-dangerous iron product may not be apparent to a toddler exploring the medicine cabinet.
Immediate Response and Treatment
Suspected iron poisoning requires immediate medical intervention, as delays in treatment significantly worsen outcomes. The poison control helpline (1-800-222-1222 in the United States) provides free, confidential guidance and should be contacted immediately when poisoning is suspected. If the victim has collapsed, experienced a seizure, has trouble breathing, or cannot be awakened, emergency services should be called without delay rather than waiting for poison control guidance.
Hospital treatment of significant iron poisoning involves several components. Whole-bowel irrigation using a special solution of polyethylene glycol may be given orally or through a stomach tube to flush remaining iron from the gastrointestinal tract. This procedure is most effective when performed soon after ingestion, before iron has been absorbed into the bloodstream. For severe cases, chelation therapy with deferoxamine—a medication that binds to iron in the blood and allows its excretion in urine—is administered intravenously. This treatment can be life-saving but requires hospitalization and carries its own risks, making prevention through secure storage the preferred approach.
Who Faces the Highest Risks
While anyone can experience adverse effects from iron supplementation, certain populations face substantially elevated risks due to their underlying health conditions, genetic factors, or life circumstances. Identifying whether you fall into a high-risk category helps determine whether iron supplementation is appropriate and what special precautions may be necessary.
Patients with Inflammatory Bowel Disease
Individuals with Crohn’s disease or ulcerative colitis occupy a particularly precarious position regarding iron supplementation. Their chronic conditions commonly cause iron deficiency through blood loss and intestinal malabsorption, creating legitimate therapeutic need for iron replacement. However, the same inflammatory processes that cause their underlying disease create tissue environments where iron-mediated oxidative damage is amplified. Research demonstrating that iron supplementation increases disease activity in Crohn’s patients confirms that standard supplementation approaches may be counterproductive in this population.
These patients require specialized management that may involve alternative iron formulations, different routes of administration, or concurrent antioxidant therapy. Intravenous iron bypasses the gastrointestinal tract entirely, potentially avoiding the mucosal damage and disease flares associated with oral supplementation. When oral iron is necessary, formulations designed for sustained release or reduced gastrointestinal contact may be preferred. Whatever approach is chosen, close monitoring for disease activity and iron status is essential to balance the benefits of correction against the risks of supplementation.
Protecting Yourself from Iron Supplement Risks
Safe iron supplementation requires attention to proper dosing, timing, storage, and monitoring. The risks documented throughout this guide can be substantially reduced through adherence to evidence-based practices that balance therapeutic benefit against potential harm.
Proper Dosing and Administration
Taking iron supplements exactly as prescribed—neither more nor less frequently than recommended—represents the most fundamental protective measure. Many patients, believing that more is better, inadvertently overdose themselves by taking additional doses when they feel tired or by combining multiple iron-containing products. Iron supplements should never be taken “as needed” for fatigue symptoms without healthcare provider guidance, as fatigue has numerous causes unrelated to iron status and excessive iron accumulation can cause serious harm.
The timing of iron doses affects both absorption efficiency and side effect profile. Most healthcare providers recommend taking iron around the same time each day to maintain consistent blood levels, with the first dose typically taken in the morning on an empty stomach for maximal absorption. Patients who experience intolerable side effects may be advised to take iron with food, understanding that this choice reduces absorption efficiency and may require longer treatment duration. Whatever schedule is chosen, consistency in timing helps optimize outcomes.
Essential Storage Safety Measures
The tragic reality of pediatric iron poisoning makes secure storage an absolute requirement for any household containing iron supplements. Iron products should be kept in their original containers with child-resistant caps properly secured after each use. Storage locations should be high enough that children cannot access them even when using furniture or countertops as stepping aids. The bathroom medicine cabinet—often the default storage location for medications—is generally unsuitable due to humidity that can damage products and the likelihood that children will find ways to access bathroom spaces.
Disposal of unneeded iron supplements requires the same care as storage. Medications should never be flushed down the toilet due to environmental concerns and potential for accidental access. Medicine take-back programs, available through many pharmacies and community organizations, provide the preferred disposal method. Patients should inquire about take-back programs in their communities and take advantage of these services when discontinuing iron therapy or discovering that supplements are no longer needed.
Iron supplement risks are real and significant, but they don’t mean that iron supplementation should be avoided when medically indicated. Rather, these risks underscore the importance of appropriate prescribing, informed patient participation, and vigilant monitoring throughout the course of treatment. By understanding how iron can cause harm, patients and providers can work together to maximize benefits while minimizing the dangers that accompany this essential but potentially toxic mineral. Always consult with your healthcare provider before starting iron supplementation, and never exceed recommended doses without medical supervision—your health depends on it.